The damaged vein condition progresses with time. Fortunately, each stage has distinguishing symptoms. Knowing the symptoms will help you determine when to seek medical attention.
If you exhibit any of the following symptoms of a venous condition, you should get diagnosed and treated right away to stop the problem from getting worse.
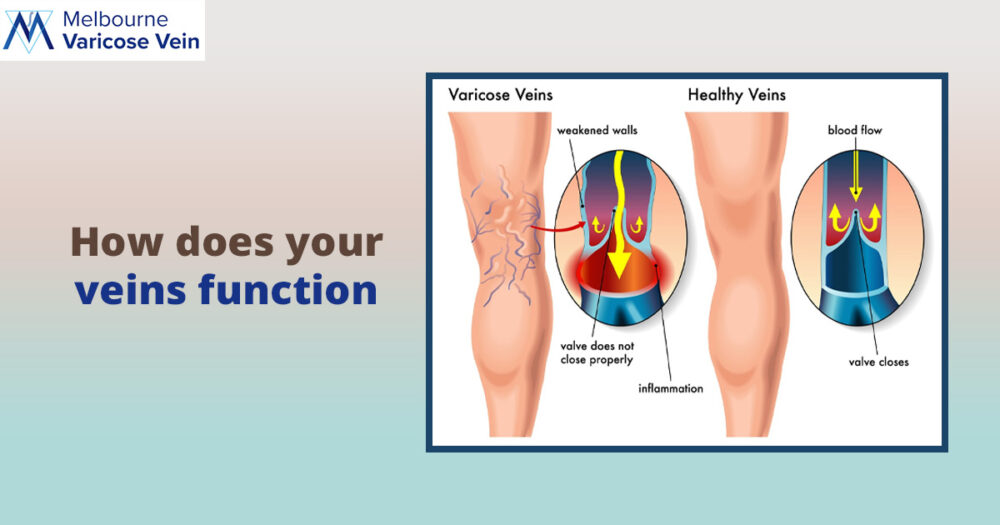
How does the vein function
The blood circulatory system has two sections. The first section is the arteries, which provide all of the body's tissues with oxygen and nourishment. The second section consists of the veins, which return oxygen-depleted blood to the heart and lungs. However, veins struggle more than other organs to do their jobs because they have to transport blood against gravity.
The movement of blood against gravity in the human body relies on two methods. First, the calf and thigh muscles contract to move the blood forward. Second, once blood passes through a series of one-way valves in a vein, the valves close.
If the vein walls or valves weaken or become damaged, blood can return to the lower limbs and pool around the weaker or damaged area. Both weakening and injury are crucial factors in high blood pressure, and they result in venous insufficiency, a condition characterized by slow flow. If you don't address the underlying issue, the condition becomes chronic.
Chronic venous insufficiency (CVI) affects about 40% of adults. The symptoms of CVI may be merely cosmetic, but they can also cause pain, aching, swelling, and more severe vein disease in its later stages. Getting treated right away is crucial because of this.
Symptoms of a vein condition
As we mentioned earlier, CVI (Chronic Venous Insufficiency) is a condition in which blood flow slows and collects in the injured vein. It can also be accompanied by skin changes, agonizing "heaviness" in the ankles and lower legs, itchy and flaky skin, and other symptoms.
Venous pressure affects the vein's wall, leading to the development of spider veins and reticular feeder veins (small, blue veins) in web-like patterns on the skin's surface. These veins often appear on the legs and, although not medically threatening, can be a symptom of an underlying disease.
Spider veins can be an underlying cause of Varicose veins. They affect the larger surface veins, leading to increased pressure inside the veins. Varicose veins are easily recognizable as large, ropy, colored swellings on the leg caused by engorged veins.
Furthermore, they can also cause a more serious disorder known as deep vein thrombosis (DVT), which results in a blood clot in a deep leg vein.
The strain on the vein walls also causes the veins to leak into the surrounding tissue, resulting in edema (swelling) in the region around the compromised vein. This can lead to itching, burning sensations, and a warm sensation in the leg when touched. It can also be painful and cause dimpling.
If left untreated, edema can alter the appearance of the skin over the affected veins, leading to a disorder known as venous stasis dermatitis. You may notice brownish-red blotches, also known as "cayenne pepper spots," on your lower legs and ankles. The discoloration is caused by hemosiderin, a byproduct of the blood's hemoglobin, which carries oxygen. The skin may also thicken, shine, or develop scales.
Venous stasis dermatitis can worsen and lead to the development of venous ulcers. These ulcers are open sores surrounded by discolored or hardened skin on the lower leg or ankle. If they get infected, they can be extremely painful, despite the sore itself not being particularly painful.
The main issue with these ulcers is that they take a long time to heal and are vulnerable to infection, especially in diabetics. More than 80% of lower limb amputations begin with foot ulcers.
If you exhibit any symptoms of a vein condition, make an appointment at Melbourne Varicose Vein Clinic right away for a thorough evaluation with Dr. Nellie.

