Varicosities are veins that have become enlarged, twisted, and weakened most commonly in the legs, but also in the pelvis and vulva. You may recognise them as the raised, rope-like or web-like lines that appear beneath the skin. They are more than a cosmetic issue. Left untreated, varicosities can cause persistent aching, swelling, skin changes, and in severe cases, venous ulcers.
In this guide, we explain what varicosities are, why they develop, the different types, and which treatments deliver lasting results — including the options available at Melbourne Varicose Vein Clinic.
Varicosities are enlarged veins caused by weakened or damaged valves that allow blood to pool instead of flowing back to the heart. They appear most often in the legs (varicose veins), but also in the pelvis (pelvic varicosities) and vulva (vulvar varicosities). They affect around 30% of adults and are more common in women.
How Do Varicosities Develop?
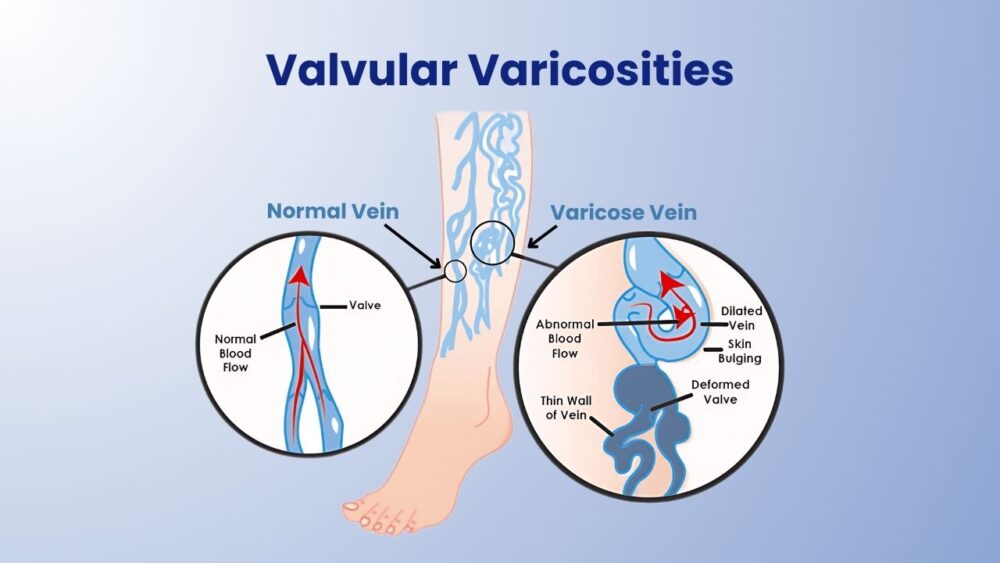
Your veins contain small flaps of tissue called valves. These valves open to let blood flow towards your heart, then close to stop it flowing backwards. When a valve weakens or breaks down, blood leaks back and pools in the vein. The vein wall stretches under this pressure, becomes enlarged and distorted and a varicosity forms.
Several factors affect how quickly valves wear out. Collagen is the structural protein in your vein walls and valves varies from person to person. If your collagen is naturally more flexible, your valves may degrade faster under normal pressure. This is partly why varicosities run in families.
Common Causes of Varicosities
- Genetics: a family history of varicose veins significantly raises your risk.
- Pregnancy: rising progesterone relaxes vein walls, and the growing uterus increases pressure on pelvic veins.
- Prolonged sitting or standing: reduced muscle movement slows blood flow and raises venous pressure.
- Previous blood clots (DVT): clots damage valves directly, causing back pressure and eventual valve failure.
- Hormonal changes: high progesterone from pregnancy or medication weakens vein walls.
- Last leg injuries or surgery: direct trauma can disrupt the valves inside affected veins.
- Obesity: extra body weight increases the load on leg veins.
Types of Varicosities: Leg, Pelvic & Vulvar
Not all varicosities look the same or appear in the same location. Understanding the type you have helps determine the right treatment approach.
Leg Varicosities (Varicose Veins)
These are the most common form. They appear as raised, blue or purple twisted veins on the calves and thighs. Leg varicosities often cause heaviness, aching, and swollen ankles particularly towards the end of the day.
Vulvar Varicosities
Vulvar varicosities affect the outer lips of the vagina and are more common than most people realise. Between 4% to 10% of pregnant women develop them and the actual number is likely higher, since many women feel too embarrassed to mention them to a doctor.
These varicosities cause visible swelling, a dull aching in the pelvic area, and pain during sex or menstruation. They also make some women feel the urge to urinate more frequently. The good news: vulvar varicosities during pregnancy usually resolve on their own within six weeks of birth.
Pelvic Varicosities
Pelvic varicosities occur in the veins surrounding the uterus and ovaries. They often go undiagnosed because the veins are not visible externally. Symptoms include chronic pelvic pain that worsens when standing or sitting for long periods, and pain that increases throughout the day.
Signs Your Vein Valves Are Damaged
As more valves fail, blood circulation in your legs deteriorates. Doctors call this venous insufficiency. It can range from mild discomfort to severe skin and tissue changes. Watch for these warning signs:
- Stinging or itchy legs especially around visible veins.
- Bulging, raised veins visible under the skin.
- Persistent aching or heaviness in the legs.
- Muscle fatigue, cramps, or leg spasms.
- Swollen ankles or feet, particularly by evening.
- Restless legs, especially when trying to sleep.
- Skin discolouration dark, bruise-like patches around the ankles.
- Venous ulcers open sores on the lower leg that are slow to heal.
If you recognise three or more of these symptoms, speak to a vein specialist. Early treatment prevents the condition from progressing to skin ulcers or deep vein complications.
How Hormones Affect Varicosities
Female hormones play a significant role in varicosity development which partly explains why women are more commonly affected than men.
Progesterone relaxes vein walls and softens the valve tissue. At high levels such as during pregnancy or with certain contraceptive medications — veins dilate and valves begin to leak. Too much progesterone can make the valve flaps so flexible that they can no longer seal shut properly.
Oestrogen has a protective, anti-inflammatory effect on vein valves. Studies show that oestrogen receptors in veins increase as venous insufficiency worsen in both men and women suggesting the body tries to compensate as valve function declines.
Varicosities Treatment Options
Treatment ranges from self-care measures to minimally invasive clinic procedures. The right option depends on the type, size, and severity of the affected veins.
Self-Care Measures
These steps reduce symptoms but do not remove existing varicosities:
- Compression stockings: medical-grade stockings prevent blood pooling and reduce swelling and ache.
- Regular walking activates the calf muscle pump, pushing blood back up towards the heart. Swimming and dancing offer similar benefits.
- Leg elevation: raising your legs above heart level helps gravity assist blood return.
- Avoid prolonged sitting or standing take breaks every 30–45 minutes to move your legs.
Minimally Invasive Clinic Treatments
When symptoms worsen, or if you want a permanent solution, these in-clinic procedures close affected veins with no hospital stay required:
| Treatment | How It Works | Best For |
|---|---|---|
| Sclerotherapy | A solution is injected into the vein, causing it to close and be absorbed by the body. | Spider veins & small varicosities |
| Ultrasound-Guided Sclerotherapy (UGS) | Injections guided by ultrasound reaches deeper or hidden varicosities with precision. | Larger or hidden varicosities |
| EVLA / RFA | A laser or radio-frequency probe applies heat inside the vein, sealing it permanently. | Large saphenous vein varicosities |
| Medical Adhesive (VenaSeal) | Medical-grade glue seals the vein instantly without heat. | Trunk varicosities; patients avoiding heat |
| Ambulatory Phlebectomy | Surface varicosities are removed through tiny 1mm incisions. Walk-in, walk-out. | Bulging surface varicosities |
Does Medicare Cover Varicosities Treatment in Australia?
Medicare rebates apply to varicosities that are medically necessary meaning they cause symptoms such as pain, swelling, skin changes, or ulceration. Purely cosmetic spider veins are generally not eligible. Eligible veins must typically be 2.5mm or larger in diameter.
At Melbourne Varicose Vein Clinic, we assess your eligibility during your first consultation and provide a full breakdown of costs and Medicare rebates before any treatment begins.


