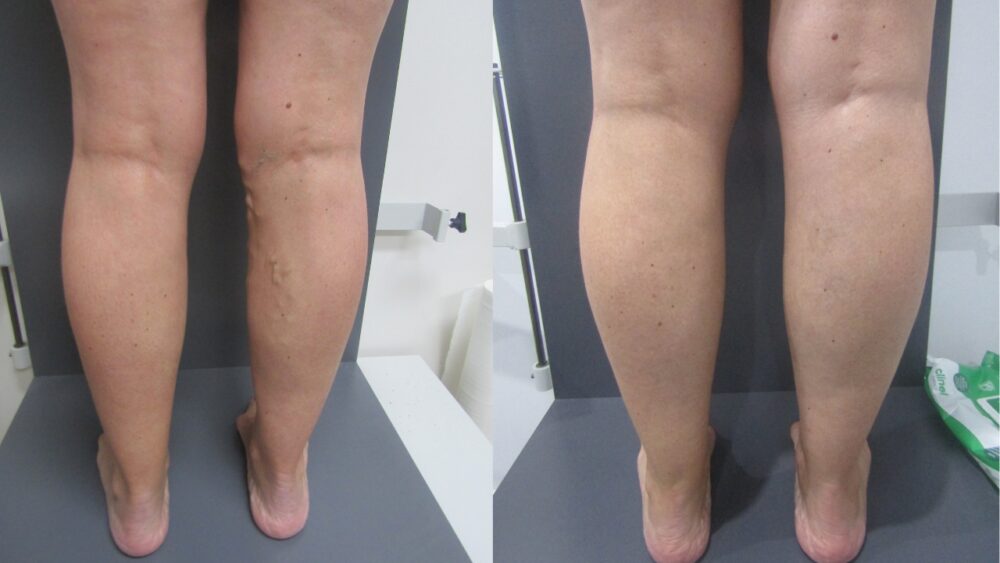
A 60-year-old woman with a 15-year history of right lower leg varicose veins presented with ongoing symptoms of leg heaviness and discomfort, particularly with prolonged standing. The veins had progressed following pregnancy. Using EVLA to treat the Great Saphenous Vein (GSV) and ultrasound-guided foam sclerotherapy (UGFS) to address residual veins, we achieved complete symptom resolution with sustained closure at 4-year follow-up.
Varicose veins are often attributed to pregnancy, but many patients assume their symptoms will resolve after childbirth. This case demonstrates how pregnancy-accelerated varicose veins can persist into later life — and how modern minimally invasive techniques provide lasting solutions.
Pregnancy-Related Varicose Veins
The patient first noticed varicose veins in her right lower leg in her mid-40s, shortly after pregnancy. Over the following 15 years, the visible veins became increasingly prominent, and her symptoms progressively worsened.
By the time she sought treatment, she was experiencing typical symptoms of symptomatic venous insufficiency: leg heaviness and discomfort that worsened throughout the day, particularly after prolonged periods of standing. Rest and leg elevation provided temporary relief — the classic presentation of varicose veins caused by venous reflux.
The visible appearance of the veins and their progressive nature prompted her to seek specialist evaluation. She was concerned about further progression and the potential long-term implications of untreated varicose veins.
Symptoms at Initial Stage
Identifying the Source of Vein Problem
At her initial consultation, clinical examination confirmed visible varicosities along the medial right lower leg. To determine the underlying cause, duplex ultrasound imaging was performed. The ultrasound examination identified reflux (backward blood flow) in the Great Saphenous Vein (GSV), confirming that the visible surface varicosities were secondary to incompetence in this major trunk vein. The GSV, which runs along the inner thigh and calf, is the most commonly affected vein in lower leg varicose disease.
Treatment Plan: Two-Stage Approach was designed to address both the underlying reflux and the visible tributaries:
Stage 1: Endovenous Laser Ablation (EVLA)
EVLA was selected to treat the incompetent GSV. This minimally invasive procedure uses laser energy to apply heat inside the vein, causing the vein wall to collapse and seal permanently. The procedure is performed under local anesthesia as an outpatient treatment.
During the procedure, a laser fiber is inserted into the vein under ultrasound guidance. As the fiber is withdrawn, it delivers controlled heat energy, systematically sealing the entire length of the faulty vein. The sealed vein is gradually reabsorbed by the body over the following weeks and months.
EVLA is considered the gold standard treatment for GSV reflux due to its high efficacy, low complication rates, and durable results. The procedure allows the patient to walk in and walk out the same day, with minimal recovery time.
Stage 2: Ultrasound-Guided Foam Sclerotherapy (UGFS)
Following EVLA, ultrasound-guided foam sclerotherapy was performed to treat residual varicosities and venous tributaries not addressed by the primary procedure. In foam sclerotherapy, the injected solution is mixed with air or CO₂ to create a foam, allowing it to displace blood and contact more of the vein wall, improving efficacy.
This two-stage approach — targeting the main incompetent vein and its branches — provides comprehensive treatment and reduces the likelihood of residual symptoms or recurrence.
Post-operative care focused on supporting vein closure and managing normal post-procedure swelling
In the immediate post-procedure period, the patient experienced significant clinical improvement:
These early improvements are typical and occur as the sealed veins begin to reabsorb and swelling resolves. Most patients experience the majority of their symptom relief within the first two to four weeks.
The 4-Year Follow-Up
The patient returned for follow-up assessment four years after her initial treatment. This extended follow-up is particularly valuable because it demonstrates the durability of the procedure over time.
At the 4-year visit, clinical examination and duplex ultrasound imaging confirmed that the treated GSV remained completely sealed with no evidence of recurrence. The varicosities had resolved completely, and no new veins had developed in the treated area.
Cosmetically, the previously visible veins had faded significantly. The skin appearance had normalised, and the patient was able to wear any clothing without concern about appearance — a significant quality-of-life benefit beyond symptom relief.
Why 4-Year Follow-up Matters: Long-term follow-up demonstrates that EVLA is not a temporary fix. Studies show that endovenous ablation techniques have closure rates exceeding 95% at 5-year follow-up. This patient's 4-year result is consistent with published evidence supporting EVLA as a durable, definitive treatment for varicose veins — not merely symptomatic relief.
Functional and Quality-of-Life Improvements: Beyond the clinical and cosmetic outcomes, the patient reported significant improvements in her quality of life:
Complete resolution of leg pain and heaviness enabled her to return to normal activities without limitation She was able to resume exercise and physical activity, improving her overall fitness and health Freedom from cosmetic concerns allowed her to wear clothing of her choice without self-consciousness The permanent nature of the treatment provided peace of mind, knowing the condition would not recur.


