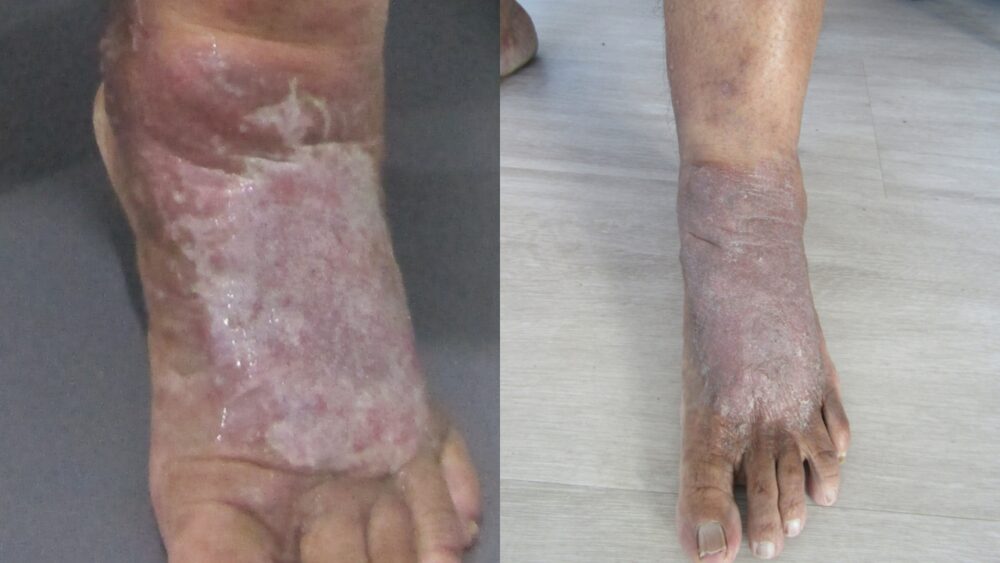
A 50-year-old woman with a 30-year history of progressive varicose veins presented with significant functional impairment: leg pain, swelling, and a venous ulcer on the left foot that prevented normal walking. Using a combination of Endovenous Laser Ablation (EVLA) and ultrasound-guided sclerotherapy, we achieved complete symptom resolution and ulcer healing within four weeks.
Varicose veins are often dismissed as a cosmetic concern, but this patient's journey illustrates how untreated venous insufficiency progresses to serious complications — and how timely intervention restores quality of life.
The Long Road: 30 Years of Progressive Symptoms
Our patient first noticed varicose veins in her 20s but chose not to pursue treatment. Over three decades, her condition worsened progressively. By the time she attended Melbourne Varicose Vein Clinic, the impact on her daily life was substantial.
She reported a range of symptoms characteristic of advanced venous insufficiency: persistent leg heaviness and aching, visible bulging veins on both thighs and calves, significant lower limb swelling, and, most concerning, a non-healing ulcer on her left foot. The pain and swelling had become so severe that she could no longer wear shoes or walk without significant discomfort.
The functional limitation had secondary health consequences. Unable to exercise due to pain, she had gained weight over time. This additional weight increased the load on her leg veins, accelerating the condition's progression: a common cycle in untreated varicose vein conditions.
Symptom Severity
Clinical Assessment and Diagnostic Findings
At her initial consultation, duplex ultrasound imaging was performed to identify the underlying cause of her varicosities and determine the best treatment approach. The ultrasound revealed reflux (backward blood flow) in three major venous systems:
This multi-system venous reflux was responsible for both the visible varicosities and the progressive skin damage that led to ulceration. The venous ulcer itself was localised to the left foot, consistent with the severity of reflux in the left lower extremity.
Treatment Plan: A Multi-Modal Approach
A comprehensive treatment strategy was developed to address both the underlying reflux and the superficial venous tributaries:
Phase 1: Endovenous Laser Ablation (EVLA)
EVLA was selected to treat the primary incompetent veins (GSV, AAGSV, and SSV). This minimally invasive procedure uses laser energy to heat and seal the faulty vein from the inside, redirecting blood flow to healthier veins.
The procedure was performed under local anaesthesia as an outpatient treatment, allowing the patient to walk in and walk out the same day. Because the vein is sealed rather than removed, it is gradually absorbed by the body over the following weeks.
Phase 2: Ultrasound-Guided Sclerotherapy (UGS)
Following EVLA, the patient underwent five sessions of ultrasound-guided sclerotherapy to treat residual varicosities and venous tributaries not addressed by the primary procedure. UGS allows the clinician to visualise the vein on ultrasound while injecting a solution that causes the vein wall to collapse and seal.
This two-pronged approach — targeting both the main incompetent veins and their branches — is considered the gold standard for comprehensive treatment of the advanced varicose vein condition.
Post-operative care focused on promoting healing and preventing complications:
Transformation at follow-up was substantial. All major symptoms had resolved:
At four weeks, the results were already impressive. Continued improvement is expected at the eight-week and six-month follow-up appointments. The sealed veins will be completely reabsorbed over the following months, and the new skin forming over the previously ulcerated area will continue to strengthen.
Post-Treatment Skin Changes: What to Expect
Long-standing varicose veins and ulceration cause lasting changes to the skin. After treatment, some changes may persist or develop:
Post-Inflammatory Hyperpigmentation: Approximately 5% of patients experience temporary brown or dark discolouration around treated veins. This typically resolves within 12 months as the skin fully heals.
Residual Pigmentation from Chronic Ulcer: In this case, some residual skin discolouration may persist due to the prolonged duration of the untreated ulcer and the associated chronic inflammatory changes to the dermal tissue. This is a normal result of chronic venous ulceration and does not indicate treatment failure. As new skin forms over the healed ulcer site, the appearance continues to improve. Specialised topical treatments (such as prescribed healing creams) support this process and promote optimal cosmetic recovery.
Key Lessons From This Case
Early Detection and Treatment Matter: This patient's 30-year delay in seeking treatment allowed her condition to progress from cosmetic concern to functional disability and tissue damage. Earlier intervention would have prevented these complications entirely.
Untreated Varicose Veins Are Progressive: Varicose veins do not improve without treatment. Left untreated, they worsen over time, increasing the risk of swelling, skin changes, and ulceration. Early treatment prevents these complications.
Quality of Life Matters: Beyond the medical benefits, this patient regained the ability to walk, exercise, and wear the shoes she wanted. The psychological and lifestyle impact of effective treatment is as important as the clinical outcomes.
Expert Assessment Is Essential: The detailed duplex ultrasound imaging identified exactly which veins were faulty, allowing for precise, targeted treatment. A comprehensive assessment is critical for planning effective, minimally invasive treatment.


